Transdermal patches have transformed how medications reach the bloodstream, offering steadier delivery and greater convenience than many oral options. From traditional skin patches to modern advanced systems, this delivery method bypasses the digestive tract and can reduce peaks and troughs. Understanding how transdermal patches work helps patients appreciate the advantages of this skin-delivery method. Different types of transdermal patches are designed for various drugs and durations, balancing release rate and skin compatibility. Evidence of transdermal patch efficacy varies with drug, design, and individual factors, while awareness of transdermal patch side effects supports safer use.
In simple terms, these adhesive skin delivery systems place medication on the surface to diffuse into the bloodstream, offering a non-oral route. These devices rely on controlled permeation principles, where the drug slowly passes through the outer skin layers using reservoir or matrix designs that regulate release. Beyond the phrase transdermal patches, you will see terms like skin patches, percutaneous patches, and topical adhesive systems that describe the same dermal delivery method. The overarching goal is to provide steady systemic exposure, avoid first-pass metabolism, and minimize local irritation through smart material choices and proper site rotation. As science advances, these dermal delivery platforms expand into diverse indications and new drug classes, supported by smarter adhesives and personalized dosing approaches.
What Are Transdermal Patches and Why They Matter for Medication Delivery
Transdermal patches have evolved from basic medicated bandages into sophisticated delivery systems that place medication on the skin and release it steadily into the bloodstream. This approach helps maintain consistent drug levels over hours or days, reducing the peaks and troughs that can accompany some oral therapies. For patients, patches offer convenient, discreet wear and the potential to bypass the digestive system, which can lessen certain gastrointestinal side effects and variability in absorption.
While many people associate transdermal patches with nicotine replacement or pain relief, these devices actually span a wide range of uses, including hormone therapy, antiemetic relief, and cardiovascular or neurological medications. Understanding this technology empowers patients to anticipate when a patch should be replaced, recognize signs of insufficient effect, and discuss alternatives with a healthcare provider.
How Transdermal Patches Work: Permeation, Release, and Skin Interactions
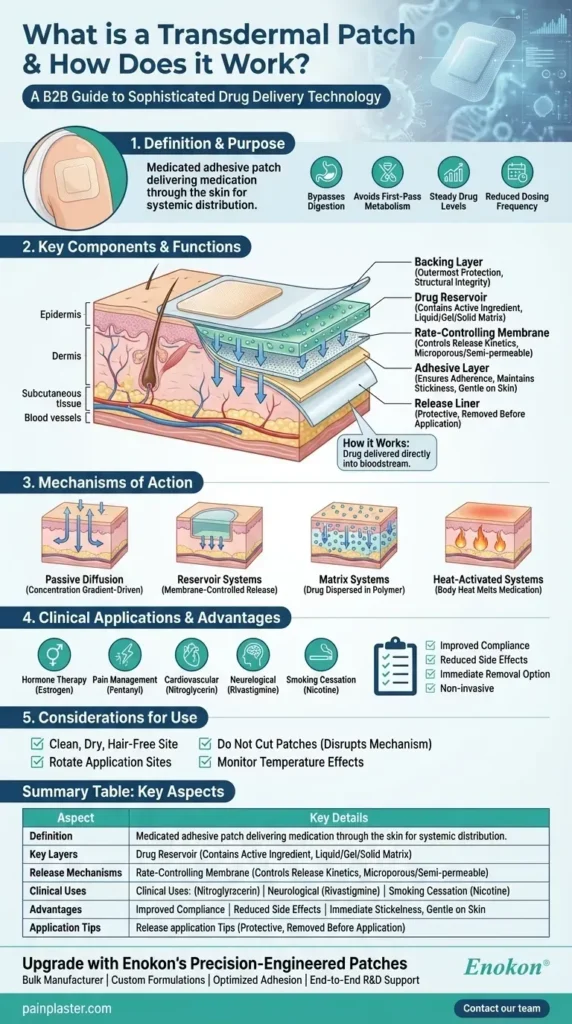
How transdermal patches work combines skin biology with clever engineering. The skin’s outer barrier, the stratum corneum, limits drug entry, so modern patches rely on permeability enhancers, optimized formulations, and device designs that favor diffusion into the underlying tissues.
To tailor release, patches come in different designs. Reservoir patches hold drug in a separate layer and use a rate-limiting barrier, while matrix patches disperse the drug through a polymer matrix. The drug-in-adhesive variant places medication directly in the adhesive layer. Understanding how transdermal patches work involves recognizing how patch design interacts with the skin to control diffusion, including reservoir, matrix, and drug-in-adhesive formats. Where you apply the patch and how long you wear it also influence how much drug reaches the bloodstream.
Types of Transdermal Patches: Reservoir, Matrix, Drug-in-Adhesive, and Multipatch Systems
Types of transdermal patches are varied, each with distinct advantages and tradeoffs. Reservoir patches place drug in a separate reservoir and release it through a controlling membrane to maintain steady delivery.
Matrix patches disperse the active ingredient through a polymer matrix and can be more flexible for different drugs. Drug-in-adhesive patches embed the medication directly in the adhesive, offering a lighter, more comfortable option, though the loading and adhesion must be balanced to ensure consistent delivery. Additionally, multipatch systems combine patches for different times of day or complementary effects, while hormone patches illustrate the broad applications beyond pain relief and antiemetics.
Evaluating Efficacy: Transdermal Patch Efficacy Across Drugs and Conditions
Transdermal patch efficacy depends on the drug’s properties, the patch design, and patient-specific factors such as skin type and site rotation. When well designed, patches can deliver a steady dose that preserves therapeutic levels and may reduce gastrointestinal variability from oral medications.
Bypassing first-pass metabolism can enhance bioavailability for certain drugs, which is a key reason some medicines perform better when delivered via patches. However, not every drug is suitable for transdermal delivery; stability, permeability, and formulation constraints limit which therapies can benefit from this method.
Managing Side Effects and Safety: Transdermal Patch Side Effects and Precautions
Transdermal patch side effects are typically related to the skin—the most common issues are local reactions such as redness, itching, or mild irritation at the application site. Allergic dermatitis can occur in sensitive individuals, often linked to adhesives or excipients. Rotating sites and ensuring clean, dry skin can help minimize irritation.
Dose-related concerns can arise if absorption is higher than expected due to skin condition or external heat. Proper patch removal, disposal, and site rotation help mitigate risks. Special populations—pregnant or breastfeeding individuals, older adults, and people with skin conditions—may require closer monitoring or alternatives to patch delivery.
Practical Guidance for Choosing, Applying, and Caring for Skin Patches
When selecting a patch, it’s important to review the drug, dose, release rate, and wear duration, and to choose an application site with clean, dry skin. Common sites include the upper arm, chest, back, or abdomen, avoiding hairy or irritated areas to improve adhesion.
Practical use includes routine pairing, monitoring skin health, and avoiding heat or moisture that can compromise adhesion. Proper storage, handling, and disposal—keeping patches out of reach of children and pets—along with caregiver education, help maximize effectiveness of skin patches and reduce accidental exposure.
Frequently Asked Questions
What are transdermal patches and how do they work?
Transdermal patches are adhesive devices that deliver drugs across the skin into the bloodstream, providing a steady release over hours or days. They bypass first-pass metabolism, which can improve bioavailability and consistency of effect. Delivery depends on patch design (reservoir or matrix), skin permeability, the drug’s properties, and the wear duration.
What are the types of transdermal patches and how do they differ from skin patches?
Common types include reservoir patches, matrix patches, drug-in-adhesive patches, multipatch systems, and hormone patches. Each design uses different release mechanisms to control drug delivery. The term skin patches covers a broad family of adhesive patches worn on the skin, including transdermal and other topical products.
How effective are transdermal patches for different medications?
Transdermal patch efficacy depends on the specific drug, patch design, and patient factors such as skin type and site rotation. Well-designed patches can provide steady drug delivery and convenient dosing, but not all drugs are suitable for transdermal delivery due to permeability and stability constraints.
What are common transdermal patch side effects and how can I minimize them?
Local skin reactions such as redness or itching are common with transdermal patches. Allergic dermatitis can occur in some individuals. To minimize issues, rotate application sites, ensure clean, dry skin, avoid applying lotions under the patch, and monitor for signs of irritation. Discontinue and seek guidance if adverse effects persist.
Who should consider transdermal patches as an alternative to oral medications?
People who benefit from steady drug levels and avoiding gastrointestinal metabolism may prefer transdermal patches. Hormone patches, nicotine replacement, and certain analgesics or antiemetics illustrate the broader range beyond nicotine. Always consult a clinician to determine if this delivery method fits your treatment.
How should I choose and use transdermal patches safely (application sites, rotation, storage)?
Choose the patch based on the drug, dose, release rate, and wear duration. Apply to clean, dry skin on sites with minimal movement; rotate locations to minimize irritation. Store patches in their original packaging in a cool, dry place away from children, and check patch integrity before use.
| Aspect | Key Points |
|---|---|
| What they are and why they matter | Adhesive devices that deliver drugs across the skin into the bloodstream, providing a steady release over hours to days with convenient, discreet wear (often bypassing some oral absorption limitations). |
| How transdermal patches work | Key factors include the skin barrier (stratum corneum), patch design (reservoir vs. matrix), drug properties (lipophilicity, molecular weight), and application site/duration, all influencing absorption and effectiveness. |
| Types of transdermal patches | Reservoir patches, matrix patches, drug-in-adhesive patches, multipatch systems, and hormone patches (plus other applications like pain relief, antiemetics, etc.). |
| Evidence of efficacy | A well-designed patch aims for steady drug delivery, potential avoidance of first-pass metabolism, and improved adherence; limitations exist for drugs that don’t meet permeability/stability criteria. |
| Common side effects and safety | Local skin reactions, potential allergic dermatitis, dose-related absorption issues, proper removal/disposal, and special considerations for pregnant, elderly, or skin-condition patients. |
| Choosing and using safely | Know the drug/dose/release rate, select an appropriate site, prepare skin, rotate sites, store patches properly, and follow wear time and replacement guidance. |
| Practical tips | Establish a routine, monitor skin health, watch for heat/moisture effects on adhesion, educate caregivers/patients, and maintain overall skin health. |
| Myths vs. facts | Myth: patches release all medicine at once. Fact: most patches provide controlled, gradual release. Myth: patch pain means failure. Fact: mild site discomfort can occur; persistent pain needs clinician input. Myth: patches are only for nicotine replacement. Fact: many drugs use transdermal delivery. |
| Future directions | Advances in permeation, smarter adhesives, micro-needling-assisted delivery, and personalized patch designs to broaden usable drugs and indications. |